Subchondroplasty
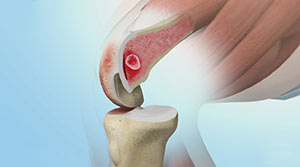
Knee osteoarthritis (OA) is a common form of arthritis that causes joint pain and stiffness. It is a progressive disease in which the joint cartilage gradually wears away and may lead to disability.
Bone marrow lesions or BMLs are strong predictors of osteoarthritic cartilage damage. Bone marrow lesions are visible on an MRI but not in a regular X-ray. BMLs are sites of chronic inflammation of subchondral bone. They lie below the bone surface within the marrow and are accompanied by swelling and fluid collection (edema). BMLs are associated with subchondral defects, insufficiency fractures and stress fractures.
Conservative treatments for BMLs include pain medications, knee braces, crutches, and physical therapy. However, long lasting (chronic) BMLs that do not heal by themselves will require treatment. Patients with chronic BMLs have faster cartilage destruction and are more likely to require a total knee replacement, earlier.
Subchondroplasty is a minimally invasive procedure that is performed to specifically repair chronic BMLs by filling them with a bone substitute material. The bone substitute is then slowly resorbed and replaced with healthy bone repairing the bone defect. Subchondroplasty also resolves the associated edema. Subchondroplasty may be performed alone or along with other arthroscopic procedures.
Ideal Candidate
Patients diagnosed with BMLs as the primary source of pain in the knee may benefit from the procedure. However, subchondroplasty is contraindicated in patients with BMI more than 40 or those with severe malalignment of the knee joint.
Procedure
The whole subchondroplasty procedure is performed under fluoroscopy to accurately target the chronic BMLs. Fluoroscopy provides the surgeon with intraoperative real time X-ray images of the surgical area to guide the surgeon. Before the procedure, the BMLs are first diagnosed on a T2 Fat Suppressed MRI.
- For subchondroplasty, first, the patient is administered general anesthesia.
- A semi-circular reference frame is placed relative to the individual patient’s tibia or shin bone. The semi-circular frame allows the surgeon to target the internal subchondral location of BML from a range of trajectories. A pin is inserted through the skin to the bone under fluoroscopic imaging using this semi-circular frame.
- A cannulated drill is then used to advance the pin to the desired depth in the bone.
- The semi-circular guide is then removed leaving only the pin.
- A cannula is placed over the pin and is slid into the bone until it is firmly in place.
- The luer lock of the delivery syringe filled with the bone substitute is attached to the back of the cannula.
- The bone substitute is then injected into the bone by applying steady pressure. The delivery syringe is then detached. If more bone substitute is required an additional filled syringe may be attached to the same cannula and injected until the desired volume is reached.
- A trocar is inserted into the delivery cannula to push the left behind bone substitute into the bone.
- The cannula is then removed.
- Finally, proper placing of the bone substitute is confirmed using the fluoroscopic imaging and the incision is closed.
After the Procedure
Some pain and discomfort in the operated area is usually experienced for 1-2 days after the procedure. Pain medications will be prescribed to manage it. Crutches will be recommended for 1-2 weeks after the surgery to reduce weight bearing on the operated leg. Physical therapy will also be recommended to regain strength and mobility in the knee.
Advantages of Subchondroplasty
Subchondroplasty is a minimally invasive procedure with the following advantages:
- It is an outpatient procedure. The patient is usually discharged on the same day as the surgery.
- It leads to faster recovery and quicker return to normal activities.
It does not hinder total knee replacement if required in the future.









